One of the biggest challenges in cancer care is that the same therapy can be highly effective for some patients yet fail entirely for others. A new study published in Nature Communications, led by Dr. Louise Fets at the MRC Laboratory of Medical Sciences (LMS), takes a closer look at why this happens. The researchers focused on PARP inhibitors, a class of targeted cancer drugs, and tracked how they move through ovarian tumor samples using advanced imaging tools.
Their findings show that these drugs can accumulate inside lysosomes, small structures within cells that act as “recycling centers.” Once inside, the drugs can become trapped and later released, influencing how well the treatment performs.
Mapping How Cancer Drugs Spread Inside Tumors
Cancer treatment options have expanded rapidly in recent years, improving outcomes for many patients. PARP inhibitors, in particular, have transformed care for ovarian cancer. However, not all patients benefit, and some develop resistance over time. For these drugs to work, they must build up inside cancer cells at levels high enough to trigger cell death. Despite this, scientists still have limited understanding of how drugs distribute within tumors and what controls that process.
This research shows that effectiveness depends not only on whether a drug reaches a tumor, but also on how it spreads within it and inside individual cells. To study this, researchers used thin slices of ovarian tumors taken from patients and kept alive in the lab. These samples, known as “explants,” were treated with PARP inhibitors so scientists could directly observe how the drugs moved through real human tumor tissue.
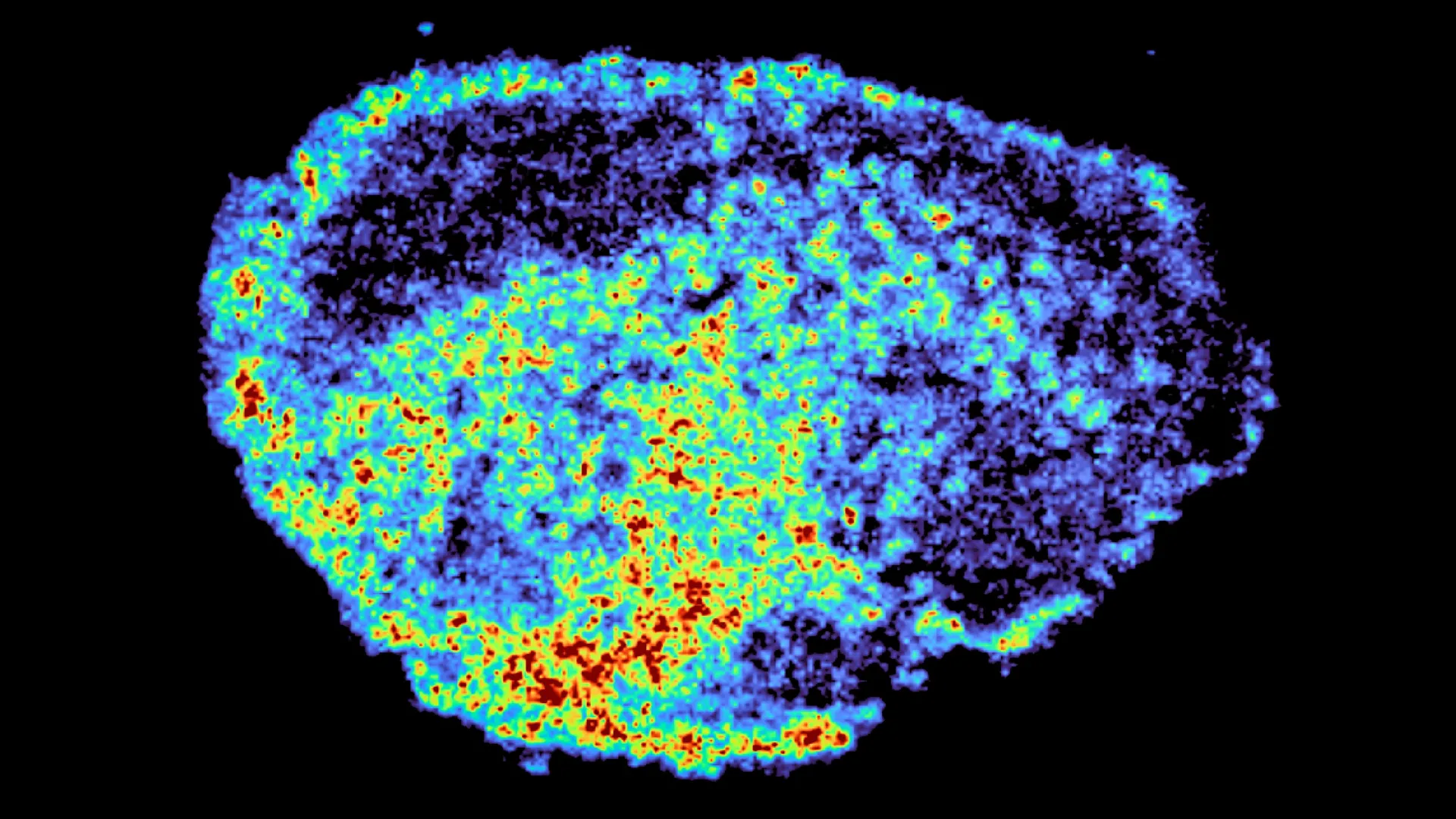
Using mass spectrometry imaging, the team produced detailed maps showing exactly where the drugs accumulated. They paired this with spatial transcriptomics, which allowed them to examine gene activity in areas with high and low drug levels within the same sample. The results revealed striking differences in drug distribution, both within individual tumors and between patients, even when the same dose was used.
“A novel aspect of this study was the use of mass spectrometry imaging to directly measure and visualize drug uptake in patient tumour tissue. Through the spatial mapping of drug molecules, we could pinpoint regions of high and low drug and compare gene expression, from the same tissue slice, using spatial transcriptomics,” says Dr. Zoe Hall, senior author and Associate Professor at Imperial’s Department of Metabolism, Digestion and Reproduction.
Lysosomes Act as Hidden Drug Reservoirs
The researchers discovered that lysosomes play a central role in this uneven distribution. Some PARP inhibitors are drawn into these compartments and stored there instead of spreading evenly throughout the cell. This creates internal pockets where drugs accumulate.
These lysosomes act as slow release reservoirs — holding onto the drug and releasing it gradually — which increases exposure in certain cells while leaving others with much lower levels. Not all PARP inhibitors behave in the same way. The study found that drugs like rucaparib and niraparib are affected by this process, while others such as olaparib are not.
“We were surprised to see large variability in drug accumulation at the single-cell level. This variability was driven by the build-up of a drug in lysosomes, which are acting as reservoirs, increasing the exposure of cancer cells to drugs, by storing and releasing the drug when needed,” says Dr. Carmen Ramirez Moncayo, first author and Postdoctoral Researcher at the LMS.
What This Means for the Future of Cancer Treatment
PARP inhibitors are already widely used to treat ovarian, breast, and prostate cancers, and they are being tested in many other cancer types. Gaining a better understanding of how these drugs are stored and distributed inside cells could lead to more personalized treatment strategies, improving effectiveness while reducing resistance and relapse.
“By understanding how drugs are taken up into cells, we can understand whether this influences why cancer drugs work for some people and not for others. Eventually, we hope to be able study the molecular signature of a patient’s tumor to help to tailor therapeutic approaches in a more personalized way,” says Dr. Louise Fets, senior author and Head of the LMS’ Drug Transport and Tumour metabolism Group.
This study was conducted using tumor tissue maintained outside the body. In real patients, drugs are delivered through the bloodstream, and tumor blood vessels are often disorganized, which may further contribute to uneven drug distribution. Future studies will use animal models and larger patient groups to better understand how drug delivery, tumor structure, and lysosomal storage interact in clinical settings, including in relapsed cancers.
This research was supported by funding from the Medical Research Council, Cancer Research UK, a PhD studentship from the Integrative Toxicology Training Partnership administered by the MRC Toxicology Unit, and a Victoria’s Secret Global Fund for Women’s Cancers Career Development Award, in partnership with Pelotonia and AACR.